By Erin Maxwell || Layout Assistant
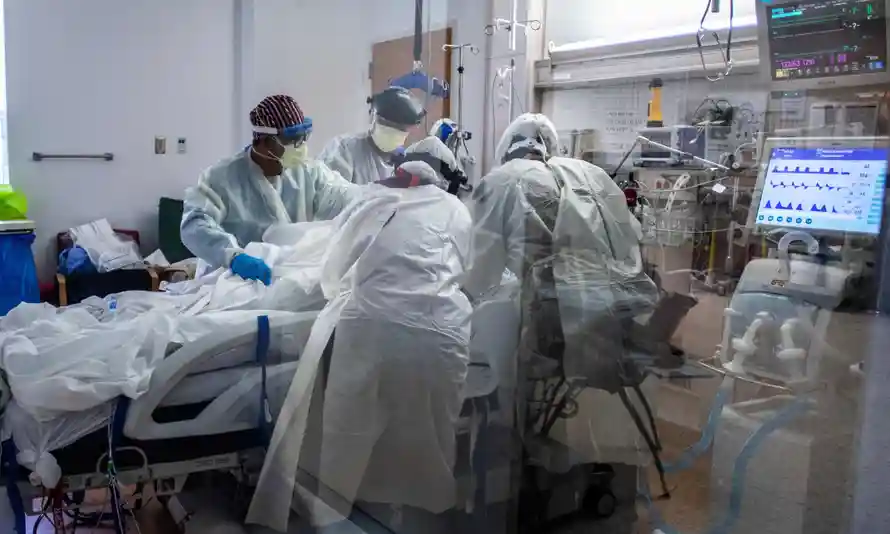
As an RNA virus, mutations leading to new variants of the coronavirus tend to appear once or twice a month, usually without a major change to the virus’s behavior. However, in early December, the Government Chief Scientific Adviser of the United Kingdom, Sir Partick Vallance, officially announced a threatening new strain, genomically named SARS-CoV-2 VUI 20212/01, which has been responsible for an astronomical rise in the United Kingdom’s infection and hospitalization rate.
What makes this mutation different is the area of the virus it alters; the characteristic spike protein on the surface of the virus is what allows it to “stick” to human cells, both inside the nose and mouth, and the internal system. This particular mutation has somehow made this spike more effective, with research indicating that it may be 70% more transmissible than the previous version of the virus. Although the mutation has been genomically proven to be more transmissible, there is no evidence that its severity is higher. Patrick Vallance, the British Chief Scientific Adviser, suggested that this mutation “moves fast, and is becoming the dominant variant” (CBS News). In response to this mounting threat, Boris Johnson has put the country in a lockdown whose scale echoes early Spring 2020, placing millions under Tier 4 restrictions.
Across the ocean, a similar variant has first been detected in Columbus, Ohio, and named COH.20G/501Y. Like the UK strain, this variant is much more transmissible, but the prevalence of the strain in the United States has not yet been measured. As of this week, this variant containing 17 distinct genetic changes has been found in nine states, multiplying alongside geographically similar viruses in Brazil, South Africa, Nigeria, and Australia. Although the exact scientific reason for the increasingly contagious trend is yet to be determined, scientists are cautioning government officials to take increased action to prevent an explosion of cases.

This news comes at a fragile time for many countries, as daily records continue to be set and hospital systems are strained to the point of exhaustion. Although scientists have agreed that there is no evidence suggesting that the Pfizer or Moderna vaccines will not be effective against this virus, vaccine rollout remains slow, forcing healthcare leaders to rely upon the same strategies we have been practicing since last March. Marc Lipsitch, an epidemiologist from Harvard’s Medical School suggests that even though countries should not overreact, “it’s a big deal for a world that’s already stretched trying to keep in control the old variant” (Vox). Dean Ashish Jha, of the Brown School of Public Health, shares this concern, stating that “without aggressive action to limit the spread of the virus, bolster health care systems around the country, and accelerate vaccine administration, Los Angeles offers a preview of what many communities are likely to experience over the coming months” (WebMD).
Much of the United States’ response to this variant and the pandemic in general remains in the balance as the beginning of the Biden administration promises a sharp change from the previous administration’s strategy. As additional information on these geographically different, yet genetically similar variant strains continues to disseminate, the best advice scientists currently have for the public is to simply “act like you have the virus” (Time).
Sophomore Erin Maxwell is a Layout Assistant for the News section. Her email is: emaxwell@fandm.edu.